|
|
Bad Breath
What causes bad breath?
Bad breath...halitosis, whatever you call it, it's something almost all of us suffer from at some point in our lives. So what causes this timeless turnoff, and what can be done about it?
Causes of bad breath
The odor is caused by wastes from bacteria in the mouth, the decay of food particles, other debris in your mouth and poor oral hygiene. The decay and debris produce a sulfur compound that causes the unpleasant odor.
Bad breath also may occur in people who have a medical infection, diabetes, kidney failure or a liver malfunction. Xerostomia (dry mouth) and tobacco also contribute to this problem. Even stress, dieting, snoring, age and hormonal changes can have an effect on your breath. An odor that comes from the back of your tongue may indicate postnasal drip.
To eliminate bad breath, you need to eliminate some of the most common causes of it:
Bad breath...halitosis, whatever you call it, it's something almost all of us suffer from at some point in our lives. So what causes this timeless turnoff, and what can be done about it?
Causes of bad breath
The odor is caused by wastes from bacteria in the mouth, the decay of food particles, other debris in your mouth and poor oral hygiene. The decay and debris produce a sulfur compound that causes the unpleasant odor.
Bad breath also may occur in people who have a medical infection, diabetes, kidney failure or a liver malfunction. Xerostomia (dry mouth) and tobacco also contribute to this problem. Even stress, dieting, snoring, age and hormonal changes can have an effect on your breath. An odor that comes from the back of your tongue may indicate postnasal drip.
To eliminate bad breath, you need to eliminate some of the most common causes of it:
|
Infected Gums
This can be one of the most obvious causes of bad breath. To get gums back into shape, brush thoroughly and often with a soft-bristle brush, and get into the habit of regular flossing. Your dentist can advise you of the appropriate treatment for all dental problems. |
Dirty teeth
"There are more animals living in the scum on a man's teeth," claimed a 17th-century scientist, "than there are men in a whole kingdom." Whether or not there is any truth in this, teeth can certainly collect their fair share of odor-producing debris. Best for keeping oral bacteria to a minimum is frequent brushing (with or without toothpaste) or even just swishing the mouth with water. |
|
A dirty tongue
Many dentists believe that keeping a clean tongue may be even more effective at arresting offensive breath than keeping teeth clean. Tongue-brushing is something the ancient Romans did regularly; Mohammed also encouraged his followers to practice the custom. Brush very gently, with a soft-bristle brush and keep away from the very back of your tongue as this may cause a gagging reaction. Smoking
Because it sours the mouth and disrupts digestion, smoking has been linked to bad breath for centuries. Chewing tobacco can also foul the breath. Sore, puffy, bleeding gums
Gum disease, also known as periodontal disease, is an infection of the gums surrounding your teeth. Gum disease is one of the top reasons for tooth loss in adults, and because it is virtually pain-free, many patients do not know they have the disease. During each regular checkup, your dentist will check for signs of periodontal disease by measuring the space between your teeth and gums. |
An empty stomach
Yes, skipping meals can cause foul breath as it reduces the production of saliva needed to flush away bacteria from teeth, tongue and gums. Stress can also lead to a dry mouth, which can cause double trouble when coupled with the increase in stomach acid that stress can cause. Chewing gum and lozenges can step up saliva flow, as can between-meal snacks such as fresh fruits and vegetables. Overuse of mouthwashes
Ironic as it may sound, mouthwashes may actually worsen a bad breath problem by irritating oral tissue, although it does mask bad odors temporarily. For an emergency pick-up, try a quick rinse with a mix of water and a few drops of peppermint oil. |
Gum Disease
WHAT CAUSES GUM DISEASE?
Gum disease is caused by a buildup of plaque (a sticky form of bacteria that forms on the teeth). If the plaque is not removed (by flossing, brushing, and regular dental checkups), it will continue to build up and create toxins that can damage the gums. Periodontal disease forms just below the gum line and creates small pockets that separate the gums from the teeth. Periodontal disease has two stages: gingivitis and periodontitis.
· Gingivitis -- This is the early stage of gum disease, when the gums become red and swollen, and bleed easily. At this stage, the disease is treatable and can usually be eliminated by daily brushing and flossing.
· Periodontitis -- If left untreated, gingivitis will advance into periodontitis, and the gums and bone that support the teeth will become seriously and irreversibly damaged. Gums infected with periodontitis can cause teeth to become loose, fall out, or be removed by a dentist.
CERTAIN FACTORS CAN INCREASE A PATIENT'S RISK OF DEVELOPING PERIODONTAL DISEASE, INCLUDING:
WHILE IT IS POSSIBLE TO HAVE PERIODONTAL DISEASE AND NOT KNOW IT, SOME SYMPTOMS CAN INCLUDE:
TREATING GUM DISEASE
Treatments for gum disease can vary depending on the severity of each individual case. Typical treatments include:
PREVENTING GUM DISEASE
Regular dental checkups and periodontal examinations are important for maintaining your health and the health of your smile. You don't have to lose teeth to periodontal disease, and by practicing good oral hygiene at home, you can significantly reduce your chances of ever getting gum disease. Remember to brush regularly, clean between your teeth, eat a balanced diet, and schedule regular dental visits to help keep your smile healthy.
Gum disease is caused by a buildup of plaque (a sticky form of bacteria that forms on the teeth). If the plaque is not removed (by flossing, brushing, and regular dental checkups), it will continue to build up and create toxins that can damage the gums. Periodontal disease forms just below the gum line and creates small pockets that separate the gums from the teeth. Periodontal disease has two stages: gingivitis and periodontitis.
· Gingivitis -- This is the early stage of gum disease, when the gums become red and swollen, and bleed easily. At this stage, the disease is treatable and can usually be eliminated by daily brushing and flossing.
· Periodontitis -- If left untreated, gingivitis will advance into periodontitis, and the gums and bone that support the teeth will become seriously and irreversibly damaged. Gums infected with periodontitis can cause teeth to become loose, fall out, or be removed by a dentist.
CERTAIN FACTORS CAN INCREASE A PATIENT'S RISK OF DEVELOPING PERIODONTAL DISEASE, INCLUDING:
- Smoking or using chewing tobacco
- Diabetes
- Certain types of medication such as steroids, anti-epilepsy drugs, cancer therapy drugs, calcium channel blockers, and oral contraceptives
- Bridges that no longer fit properly
- Crooked teeth
- Old fillings
- Pregnancy
WHILE IT IS POSSIBLE TO HAVE PERIODONTAL DISEASE AND NOT KNOW IT, SOME SYMPTOMS CAN INCLUDE:
- Gums that bleed easily
- Red, swollen, tender gums
- Gums that have pulled away from the teeth
- Persistent bad breath or bad taste
- Pus between your teeth and gums
- Permanent teeth that are loose or separating
- Any change in the way your teeth fit together when you bite
- Any change in the fit of partial dentures
TREATING GUM DISEASE
Treatments for gum disease can vary depending on the severity of each individual case. Typical treatments include:
- Non-surgical treatments such as at-home periodontal trays, and scaling and root planing (deep cleaning)
- Periodontal surgery and laser gum surgery
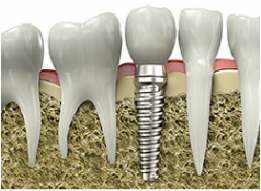
- Dental implants
PREVENTING GUM DISEASE
Regular dental checkups and periodontal examinations are important for maintaining your health and the health of your smile. You don't have to lose teeth to periodontal disease, and by practicing good oral hygiene at home, you can significantly reduce your chances of ever getting gum disease. Remember to brush regularly, clean between your teeth, eat a balanced diet, and schedule regular dental visits to help keep your smile healthy.
Toothache
For those of you who wait until something hurts to come see us, know this: Cavities do not usually hurt so waiting often increases the cost exponentially.
The average estimated cost of seeing us 2 times per year and doing one filling is $535, that’s $45 per month, or 3 gourmet coffees per week. The cost of coming to see us once every three years with a tooth ache is more like $2636, that’s $73 per month.
The average estimated cost of seeing us 2 times per year and doing one filling is $535, that’s $45 per month, or 3 gourmet coffees per week. The cost of coming to see us once every three years with a tooth ache is more like $2636, that’s $73 per month.
What could be causing my toothache?
|
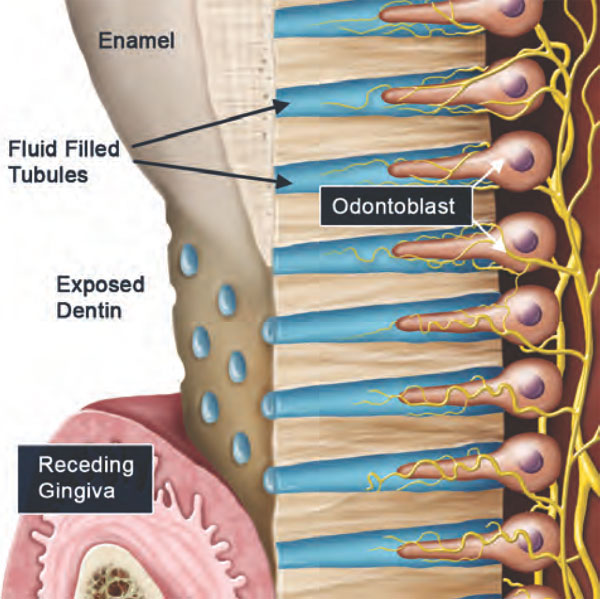
Symptom: Sensitivity to cold foods and liquids.
Possible problem: If discomfort lasts only moments, sensitivity generally does not signal a serious problem. It may be caused by an exposed root surface resulting from gum recession. Or you could just have sensitive teeth which we can address. |
Symptom: Sensitivity to hot or cold foods or drinks after dental treatment.
Possible problem: Dental work may result in tooth sensitivity due to inflammation of the pulp tissues inside a tooth. What to do: This sensitivity should last no longer then 24 hours; however, if decay has recently been removed or a filling or crown recently has been placed, a tooth may take a week or two to settle. Mild pain relievers like ibuprofen should help. If the pain persists or worsens, please call us. |
Symptom: Sharp pain when biting down on food.
Possible problem: A loose filling and/or a cracked tooth are possible causes. What to do: schedule to see Dr. Spainhower to diagnose the problem before the pain worsens. Decay will need to be removed, and a loose filling replaced by your dentist. If the pain is caused by pulp tissue damage,we may send you to an endodontist (“endo” – inside; “dont” – tooth), a specialist who will perform a root canal treatment to clean out the damaged pulp, disinfect the root canal and fill and seal the remaining space to save the tooth. A cracked tooth may be difficult to treat not only if it involves the pulp, but also depending on the location and depth of the crack. |
|
Symptom: Lingering pain after eating hot or cold foods and liquids.
Possible problem: This probably means the pulp is inflamed and/or dying, and may be irreversibly damaged usually as a result of deep decay or physical trauma. What to do: call us to see Dr. Spainhower or we will recommend you see an endodontist to diagnose the problem before the pain becomes severe due to the development of an abscess. The tooth will likely need root canal treatment to remove the dying or dead pulp tissue to save the tooth. |
Symptom: Dull ache and pressure in the upper teeth and sinus area of one or both sides.
Possible problem: Pain felt in the sinus area of the face is often associated with the upper back teeth because they share the same nerves. The origin of this “referred” pain consequently may be difficult to determine. Therefore, sinus pain can feel like tooth pain and vice versa. That's why sinus congestion from a cold or flu can cause pain in the upper teeth. Additionally it's also important to determine if clenching or grinding is a factor, as they too cause similar symptoms. What to do: schedule an appointment with Dr.Spainhower to find out if the symptoms are dentally related; otherwise, you may need to see your family physician. However, don't wait until the pain worsens. |
Symptom: Acute and constant pain from an area, but difficult to say exactly which tooth is causing the problem.
Possible problem: The pulp tissue inside a tooth is acutely infected, inflamed and dying. This is generally in response to decay coming very close to or entering the nerve. What to do: call us immediately for a thorough examination. Once the problematic tooth is isolated, a root canal treatment to remove the infected pulp tissue will bring relief while saving the tooth. Untreated, the pain could become worse. |
Symptom: Constant severe pain and pressure, swelling of the gum and sensitivity to touch.
Possible problem: A tooth may have an infection/abscess that has spread from the pulp into the surrounding periodontal tissues (“peri” – around; “odont” – tooth) and bone.
What to do: call us or an endodontist immediately. A root canal will probably be required. Over-the-counter medications like acetaminophen and ibuprofen will help minimize symptoms until you are treated.
Don't wait for the pain to get worse.
Note in the above examples, possible problems and solutions are suggested — but they only provide possible guidelines. In all cases of tooth or jaw pain or discomfort in and around the teeth and jaws, give us a call as soon as possible for a proper evaluation and treatment. We may need to refer you to an endodontist for diagnosis and treatment, especially if the issue is related to a root canal problem. And if your pain has a medical component, will refer you to a physician.
Possible problem: A tooth may have an infection/abscess that has spread from the pulp into the surrounding periodontal tissues (“peri” – around; “odont” – tooth) and bone.
What to do: call us or an endodontist immediately. A root canal will probably be required. Over-the-counter medications like acetaminophen and ibuprofen will help minimize symptoms until you are treated.
Don't wait for the pain to get worse.
Note in the above examples, possible problems and solutions are suggested — but they only provide possible guidelines. In all cases of tooth or jaw pain or discomfort in and around the teeth and jaws, give us a call as soon as possible for a proper evaluation and treatment. We may need to refer you to an endodontist for diagnosis and treatment, especially if the issue is related to a root canal problem. And if your pain has a medical component, will refer you to a physician.
TEMPOROMANDIBULAR DISORDER (TMD)
Millions of Americans suffer from chronic facial and neck pain as well as recurring headaches. In some cases, this pain is due to Temporomandibular Disorder, or TMD.
Your temporomandibular joints (TMJ) connect your lower jawbone to your skull. These joints get a lot of use throughout the day as you speak, chew, swallow, and yawn. Pain in and around these joints can be unpleasant and may even restrict movement.
SYMPTOMS OF TMD INCLUDE:
Should you notice any of these symptoms, let your doctor know. Your dentist can help indicate the presence of TMD and create an effective treatment just for you.
There are a few simple steps you can take at home or work to prevent TMD from becoming more severe, or to prevent it from occurring:
Relax your face — remember the rule: "Lips together, teeth apart" Your teeth should NEVER touch!
Your temporomandibular joints (TMJ) connect your lower jawbone to your skull. These joints get a lot of use throughout the day as you speak, chew, swallow, and yawn. Pain in and around these joints can be unpleasant and may even restrict movement.
SYMPTOMS OF TMD INCLUDE:
- Pain in the jaw area
- Pain, ringing, or stuffiness in the ears
- Frequent headaches or neck aches
- Clicking or popping sound when the jaw moves
- Swelling on the sides of the face
- Muscle spasms in the jaw area
- A change in the alignment of top and bottom teeth
- Locked jaw or limited opening of the mouth
Should you notice any of these symptoms, let your doctor know. Your dentist can help indicate the presence of TMD and create an effective treatment just for you.
There are a few simple steps you can take at home or work to prevent TMD from becoming more severe, or to prevent it from occurring:
Relax your face — remember the rule: "Lips together, teeth apart" Your teeth should NEVER touch!
Bruxism - Usually related to TMD
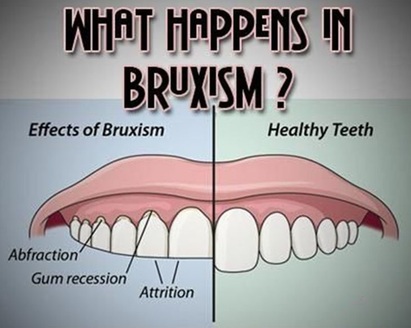
- Avoid grinding or clenching your teeth
- Don't sleep with your hand under your jaw
- Don't cradle the phone receiver between your head and shoulder — either use a headset or hold the receiver in your hand
- Chew food evenly on both sides of your mouth
- Do not sit with your chin rested on your hand
- Practice good posture — keep your head up, back straight, and shoulders squared